Newborn jaundice is common and usually harmless, but you should still watch it closely because bilirubin can rise quickly in the first days after birth. It often starts around day 2 to 4, especially if your baby is premature, feeding poorly, or has bruising or blood type incompatibility. Sunlight and water won’t treat it. Doctors use bilirubin checks and phototherapy when needed, and knowing the warning signs can help you act fast and stay reassured.
What Is Newborn Jaundice?

Newborn jaundice is a common condition in which a baby’s skin and eyes turn yellow because bilirubin builds up in the blood. You may notice this newborn jaundice between day 2 and day 4 after birth.
Bilirubin is a yellow pigment created when red blood cells break down, and your baby’s liver may not yet clear it efficiently. Most cases are mild and resolve without treatment, but you shouldn’t ignore it.
Most cases are mild and resolve without treatment, but you shouldn’t ignore it.
You can track jaundice with visual checks and a blood test that measures bilirubin levels. Careful monitoring helps you act early if levels rise.
Severe jaundice can cause complications, including kernicterus, a rare but serious injury that can lead to lifelong disability. With timely treatment, you protect your baby from irreversible brain damage. Pre-hepatic jaundice can occur in newborns due to increased bilirubin production from hemolysis.
You don’t have to accept uncertainty; clear assessment supports safer, more informed care for you and your family.
Why Newborn Jaundice Happens
You’ll see newborn jaundice when bilirubin builds up faster than your baby’s immature liver can clear it. This happens commonly in the first days of life, and it’s more likely if your baby was born early, has significant bruising, or has a blood type that’s incompatible with yours. Feeding problems and certain breast milk effects can also raise bilirubin levels, so careful monitoring helps guide treatment. Additionally, understanding the causes of jaundice is crucial for parents to ensure timely medical intervention if needed.
Bilirubin Build-Up Causes
Jaundice happens when bilirubin builds up in the blood faster than a baby’s body can remove it. In newborns, this yellow pigment comes from the natural breakdown of red blood cells, and your baby makes more of it because fetal red blood cells turn over quickly.
Most newborns develop physiologic jaundice as the immature liver catches up, often peaking around day four. If your baby has a blood type incompatibility, red blood cells can break down faster and raise bilirubin further.
Breastfeeding jaundice can also occur when poor intake lowers fluid and calorie supply, slowing bilirubin excretion. Breast milk itself isn’t the problem; low feeding is.
You can ask about treatment if jaundice seems strong, lasts, or creates concern.
Common Newborn Risk Factors
Several common factors can make jaundice more likely in the first days of life.
If your baby has premature birth, the liver may clear bilirubin in the blood more slowly, so high levels of bilirubin appear sooner.
You may also see newborns with jaundice after Rh incompatibility or ABO mismatch, which breaks down red blood cells and raises bilirubin.
Significant bruising during delivery can do the same.
In breastfed babies, breastfeeding difficulties or low intake can limit stooling and bilirubin removal.
A family history of jaundice also increases risk.
These common newborn patterns don’t mean you failed.
They help explain why some babies develop different types of jaundice and why careful monitoring supports safer, more liberated care.
Signs of Newborn Jaundice and Who’s at Risk
You may notice newborn jaundice first as yellowing of the face between days 2 and 4 after birth, with the color spreading downward as bilirubin rises.
You’re more likely to see it if your baby was born prematurely, has a blood-type mismatch with you, or had significant bruising during delivery.
Feeding problems can also raise the risk, so monitor how often your baby feeds and how many wet and dirty diapers they have. Early recognition of these jaundice symptoms is crucial for timely care.
Early Warning Signs
Watch closely in the first few days after birth, when newborn jaundice typically appears between day 2 and day 4 and often starts with yellowing of the face before moving downward.
You may notice yellow skin, yellow eyes, dark urine, or pale stools in newborns; these early warning signs suggest rising bilirubin levels.
Track feeding frequency and diaper output, because poor intake can let bilirubin stay elevated longer, especially with breast milk feeding that’s still establishing.
Premature babies have increased risk, and bruising or blood-type incompatibility can add to that risk.
If you see these changes, contact your clinician promptly. Early assessment supports timely treatment of jaundice and helps you protect your baby with calm, informed action.
Risk Factors To Watch
Some newborns are more likely to develop jaundice than others, and knowing these risk factors can help you stay alert in the first few days after birth.
You can watch for baby jaundice between days 2 and 4, when bilirubin often rises and yellowish skin may appear first on the face.
- Premature infants face a higher risk.
- A different blood type from yours can trigger red cell breakdown.
- Delivery bruising can raise bilirubin.
- Breastfeeding difficulties may limit intake and slow bilirubin clearance.
- Family history can add risk factors.
If you notice yellowing spreading downward, contact your clinician.
Early evaluation supports timely treatment and helps you protect your newborn with confidence.
When Newborn Jaundice Is an Emergency
If your newborn’s skin or eyes look more yellow, or your baby seems lethargic, feeds poorly, or is hard to wake, seek urgent care now.
Jaundice that appears in the first 24 hours after birth also needs immediate evaluation, since it often points to a pathologic cause.
Watch for high-pitched crying, irritability, or any sign of distress, which can indicate bilirubin-induced neurologic dysfunction.
You deserve clear information and timely action, and prompt treatment can prevent neurological damage.
Severe untreated jaundice can lead to permanent brain damage or, in rare cases, death.
Trust your instincts, contact your clinician right away, and don’t wait for symptoms to worsen.
Early assessment gives your baby the safest path forward and preserves healthy development.
Myths About Jaundice Treatment
A few common myths about jaundice treatment can put your baby at risk. You deserve clear facts: jaundice in newborns needs evidence-based care, not guesswork.
Sunlight isn’t an effective treatment; direct exposure can overheat your baby and cause dehydration. Phototherapy uses special blue lights and is the appropriate treatment for high bilirubin.
- Water or juice won’t lower bilirubin and may disrupt breast milk feeding.
- Herbs and tea baths don’t reach bilirubin in the body.
- Fresh goat’s milk isn’t safe; unpasteurized milk can spread infection.
- Non-medical advice can delay care your newborns need.
- Delays raise the risk of kernicterus, a preventable brain injury.
Keep breastfeeding unless your clinician tells you otherwise, because it supports bilirubin excretion. Understanding bilirubin accumulation is crucial for recognizing when to seek medical intervention.
If a remedy sounds simple but lacks evidence, treat it as a myth. You can protect your baby by choosing safe, timely care and asking a clinician about any concern.
How Doctors Treat Newborn Jaundice
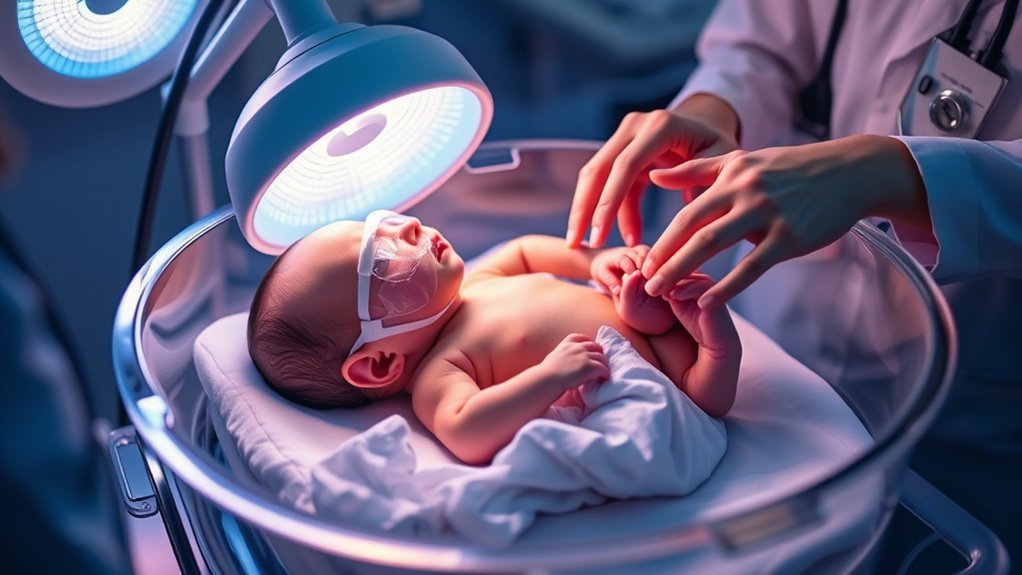
When bilirubin levels rise, doctors usually treat newborn jaundice with phototherapy, which uses special blue lights to help break down bilirubin in the skin.
You’ll usually see your newborn under this treatment in the hospital or at follow-up visits, and pediatricians track progress with blood tests and visual checks.
If bilirubin stays high, especially above 15-20 mg/dl, they may recommend an exchange transfusion to lower levels quickly and reduce complications.
Treatment plans follow age-based algorithms, so care stays timely, precise, and safe.
Keep breastfeeding during phototherapy; regular feeds help your baby pass bilirubin through urine and stool. Hydration is vital to support your baby’s overall digestive health during treatment, as it aids in bilirubin elimination.
You can ask questions, review results, and understand each step, because informed care supports confidence and protects your newborn’s freedom from preventable harm.
With prompt monitoring and the right treatment, most babies recover well and avoid serious complications.
Frequently Asked Questions
What Is an Interesting Fact About Jaundice?
An interesting fact: you’ll often see jaundice symptoms when bilirubin levels peak around day four. Your diagnosis methods guide treatment options, while breastfeeding impact, sunlight therapy, jaundice causes, risk factors, and parental concerns matter; common misconceptions persist.
What Are Some Interesting Facts About Newborns?
You’ll notice newborns sleep 16-17 hours, show infant reflexes, and communicate through cries. Breastfeeding benefits support bonding techniques, while diaper changes, skin care, baby milestones, vaccination schedule, and colic causes need your careful, reassuring attention.
What Is the Curse of Jaundice in Newborn Babies?
You’re seeing jaundice, not a curse; it’s a dramatic signal of high bilirubin levels. You’ll watch symptoms identification, jaundice causes, breastfeeding impact, risk factors, and long term effects; pediatrician advice guides treatment options, including phototherapy effectiveness.
What Is the First Color a Baby Sees?
You’ll usually see red first; your baby’s newborn vision favors visual contrast. Early development, light sensitivity, and eye development shape color perception and color recognition, while infant eyesight and perceptual abilities reach later visual milestones.
Conclusion
If your newborn looks yellow, don’t panic. Jaundice is common, and with proper monitoring, most babies recover quickly. Watch for spreading yellow color, poor feeding, or unusual sleepiness, and contact your doctor if you’re concerned. Treatment is usually straightforward, like a dimmer switch lowering bilirubin safely. By knowing the signs and myths, you can act early and help your baby stay healthy, comfortable, and well cared for from the start.
