When you’re induced, your care team starts labour with medicines or a mechanical method to trigger contractions before they begin naturally. You may feel stronger, faster contractions, and you’ll often have closer monitoring, which can limit movement but helps check your baby’s wellbeing. Induction can still end in vaginal birth, but it doesn’t guarantee an easier labour. Cervical readiness, timing, and your preferences all matter, and the details below explain what to expect.
What Is Labour Induction?
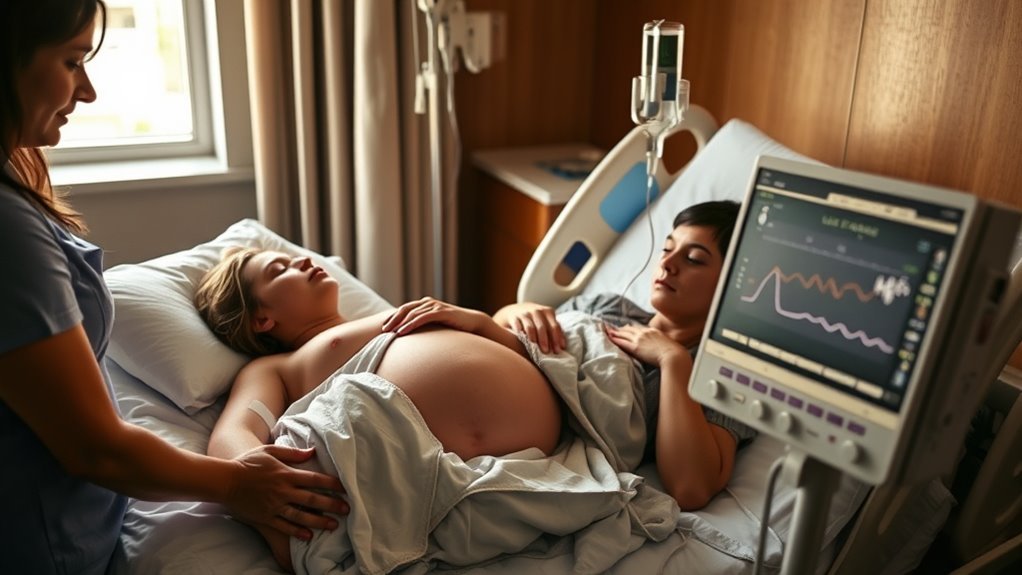
Labour induction is a medical procedure used to start uterine contractions before labour begins on its own. Your care team may induce labour with medicines such as oxytocin or with mechanical methods that support cervical ripening.
They may also use membrane sweeping or DILAPAN-S to prepare your cervix without medication. You’ll usually be offered induction after 39 weeks, but you may need it sooner if your health or your baby’s health needs closer support.
This approach doesn’t take away your agency; it’s a planned intervention designed to help you move toward birth with informed choices. Induced labour can still lead to a vaginal birth, and many people do give birth that way.
Your team will explain the method, timing, and what to expect so you can participate confidently and protect your preferences.
Why Induced Labour Feels Different
Induction can feel different because it often starts labour with artificial hormones, such as oxytocin, rather than letting contractions build on their own. In induced labor, the oxytocin hormone can trigger contractions that arrive sooner, stronger, and more sharply, so your body may have less time to adjust. This can change how you experience pain, and you may need more frequent support and pain relief.
Induction can bring stronger, sooner contractions, leaving your body less time to adjust and your pain experience changed.
- Contractions may feel more intense and less gradual.
- Monitoring may increase, which can limit movement and comfort choices.
- Your pain response can vary, so tailored support matters.
You still deserve informed, bodily autonomy-centered care. If induction is part of your plan, ask how the team will track you, explain risks, and respond to discomfort.
Clear communication can help you stay grounded and protected while labor unfolds.
What Happens During Cervical Ripening
During cervical ripening, your cervix is prepared for labor by softening and beginning to dilate, often with prostaglandin medication or a mechanical device such as DILAPAN-S.
This cervical ripening step helps your cervix shift from closed and firm to more open and flexible, so labor can start more naturally. Prostaglandins support this change and can help trigger contractions.
If you’re at least 39 weeks pregnant, your clinician may recommend cervical ripening because it can move things forward safely and often works within 24 hours.
You may also choose a membrane sweep, which separates the amniotic sac from the uterine wall and encourages your body’s own hormones.
When ripening works well, the first stage of labor may be shorter, which can mean less time waiting and more freedom in the process.
Everyone’s body responds differently, but this step is designed to support, not override, your labor.
Why Labour Induction Needs More Monitoring

When you’re induced, you’ll usually need continuous fetal monitoring so your baby’s heart rate can be checked closely for any early signs of distress.
If you’re given synthetic oxytocin, the team will watch your contractions and your response more carefully because the medication can intensify labour.
This monitoring can also limit how freely you move, so it’s important to understand the trade-off and discuss your preferences in advance.
Close Fetal Monitoring
Close monitoring is a core part of labour induction because artificial hormones such as oxytocin can intensify contractions and increase fetal stress.
During induced labour, close fetal monitoring helps you and your team see your baby’s heart rate in real time, so any sign of distress can be addressed promptly. Continuous electronic monitoring also tracks your contractions and your baby’s response.
- Detect early fetal stress
- Guide timely clinical action
- Support informed decisions
This surveillance can feel restrictive, but it’s there to keep you informed and protected.
You deserve clear explanations about why monitoring is used, what it can reveal, and how it may affect your choices. When you understand the process, you can participate more fully in informed decisions about your birth.
Restricted Labour Mobility
Alongside close fetal monitoring, induction can also limit how freely you move in labour.
When you have induction, staff often use continuous monitoring, and that can create restricted mobility. You may need to stay near equipment, which can rule out walking, swaying, or using positions that support labour progress.
This tighter monitoring can make the room feel more clinical and can increase interventions, even when you’d prefer a more physiological experience.
Limited movement may also raise pain levels and prolong labour, so your comfort matters.
If you value autonomy, ask whether monitoring can be intermittent or adapted safely.
Good induction care should balance safety with your ability to move, rest, and feel in control throughout labour.
Common Myths About Labour Induction

Labour induction is often surrounded by misconceptions, but many of these concerns don’t reflect how induction actually works. When you induce labor, you’re not giving up a natural birth; many people still achieve vaginal delivery.
- Myth: induction always needs drugs. In fact, cervical ripening can happen with non-medical methods such as DILAPAN-S, which supports opening without medication.
- Myth: your body can’t prepare itself. Hormonal shifts can mature the cervix and may still lead to spontaneous labor.
- Myth: induction is always more painful. Pain varies, and you can use effective relief options either way. You also keep control: your care team tailors the process to your situation, and you can make informed choices throughout.
These myths can limit your sense of agency; accurate information helps you participate actively, confidently, and safely in decisions about your birth.
Can You Induce Labour Naturally at Home?
If you’re wondering whether you can encourage labour at home, a few natural methods are sometimes discussed, but their effects vary.
You may hear that nipple stimulation can release oxytocin and sometimes trigger contractions, yet you should use it cautiously and stop if contractions become too frequent.
Walking, curb walking, and using an exercise ball may help you feel more comfortable or position the baby, but they don’t reliably induce labour.
Dates are often suggested because they may help soften the cervix and possibly shorten early labour, though they won’t guarantee onset.
Intercourse is also mentioned because semen contains prostaglandins, but studies haven’t confirmed that it can induce labour.
These approaches can support your body’s readiness, but none works predictably on its own.
If you want a sense of agency, discuss safe options with your clinician so you can make informed choices without pressure or myth.
Is Labour Induction Required by Law?
No—induction of labour isn’t required by law in most countries, including the UK, and you can’t be legally compelled to accept an induction date. You have rights, and knowing them helps women make clear, informed choices about birth.
Sometimes staff may present induction as mandatory; it isn’t. An induction might be recommended for clinical reasons, but recommendation isn’t coercion. Ask for the indication, the timeline, and the alternatives in plain language.
- You can decline an offered date.
- You can request reliable information.
- You can ask for time to decide.
When you understand your rights, you’re better placed to shape your birthing plan without pressure. Health professionals should explain both benefits and risks so you can give truly informed consent.
If you’re unsure, seek trustworthy guidance from midwives, obstetric teams, or evidence-based sources. That support can help women protect autonomy while making decisions that fit their values.
The Main Risks and Downsides of Induction
When you’re induced, you may notice stronger contractions and a need for closer monitoring, which can make labour feel more intense.
The benefits aren’t always certain, especially if your cervix isn’t ready, and induction can increase the chance of interventions like caesarean birth.
These risks are real, but they can be discussed clearly so you know what to expect and can make an informed choice.
Increased Pain And Monitoring
- Stronger contractions can feel less predictable and more demanding.
- Monitoring is usually stricter, which can limit movement and your options for a physiological birth.
- More interventions may follow, including epidurals or continuous fetal monitoring, adding to the overall intensity.
You still deserve clear information and choice.
Ask what support is available, how monitoring will be used, and how your preferences can guide care.
Uncertain Benefits, Real Risks
Induction can offer a clear plan, but it doesn’t guarantee a smoother or safer labor. When you’re inducing labor, synthetic oxytocin can make contractions stronger, faster, and more painful, which may increase discomfort.
Overuse of syntocinon can also stress your baby, so you deserve a careful discussion of the risks and uncertain benefits before you agree. Induction can require continuous monitoring, which may limit your physiological birth choices and make birth feel more medicalized.
It can also fail if your body or baby isn’t ready, and that isn’t a sign you’ve done anything wrong. Because induction carries possible complications and often leads to more interventions, ask your provider for clear evidence, honest options, and support that respects your autonomy and safety.
Why Some Inductions Fail
Some inductions fail because your body isn’t yet ready for labor, and that readiness depends on factors like cervical favorability and the baby’s position.
In an induction, cervical readiness matters because an unripe cervix resists change, and psychological factors like stress can blunt contractions. You may need more time before labor can begin naturally, and that’s not a personal failure.
- Timing: inducing too early often lowers success.
- Readiness: poor cervical ripening can block progress.
- Health: co-morbidities or age-related risks can complicate labor.
About 20% to 30% of inductions don’t end in vaginal birth and may require cesarean delivery.
Clinically, this reflects physiology, not blame. You deserve clear information and real choice, not pressure.
When your body and the induction don’t align, labor may stall despite careful care.
How To Make A Better Induction Decision
Because a better induction decision starts with clear information, you should review both medical and non-medical options with your provider, including how each method works, what it may change in your labor, and whether it fits your values and birth goals.
Ask your healthcare provider about benefits, risks, timing, and alternatives so you can compare choices without pressure. Induction isn’t legally required in most countries, so you have the right to ask questions, delay, or decline if the plan doesn’t feel right.
Ask about benefits, risks, timing, and alternatives so you can compare choices without pressure.
Understand that induction can increase pain and raise the chance of extra interventions, which may affect your experience. If you’re exploring natural methods, such as nipple stimulation or intercourse, discuss safety and realistic expectations first, because results vary.
Strengthen your decision by reading reputable books, seeking community support, and weighing evidence against your own priorities. When you choose with knowledge, you protect your autonomy and your birth space.
Frequently Asked Questions
Are Inductions Really That Bad?
No, inductions aren’t inherently bad. You’ll weigh induction benefits against natural alternatives, and your patient experiences matter. With individualized timing, many people still deliver vaginally, while clinicians can manage discomfort and monitor safety closely.
What Is the 5 1 1 Rule for Labor?
The 5-1-1 rule means you’ll go in when contractions are 5 minutes apart, last 1 minute, for 1 hour. You’re balancing contraction timing, labor signs, and pain management, choosing timely care, not panic.
Why Do Most Inductions Fail?
Most inductions fail because your cervix isn’t ready, so contractions don’t open it well. Induction success rates vary with your health and timing. Natural labor benefits can guide patient decision making, and you’re still in control.
Why Do Obgyns Push for Induction?
You’re getting induction because doctors follow medical guidelines, weigh induction reasons like hypertension or overdue pregnancy, and respect patient preferences. In a moonlit telegram, they aim to reduce risks and help you deliver safely, not control you.
Conclusion
You now know what induction really involves: cervical ripening, closer monitoring, and sometimes a longer, more complex process than you expected. If your induction isn’t medically urgent, you can weigh the benefits and risks with your clinician. A clear plan helps you feel grounded, like a map in unfamiliar weather. Remember, induction isn’t automatically safer or easier; it’s a medical tool that works best when it matches your needs, timing, and health.
