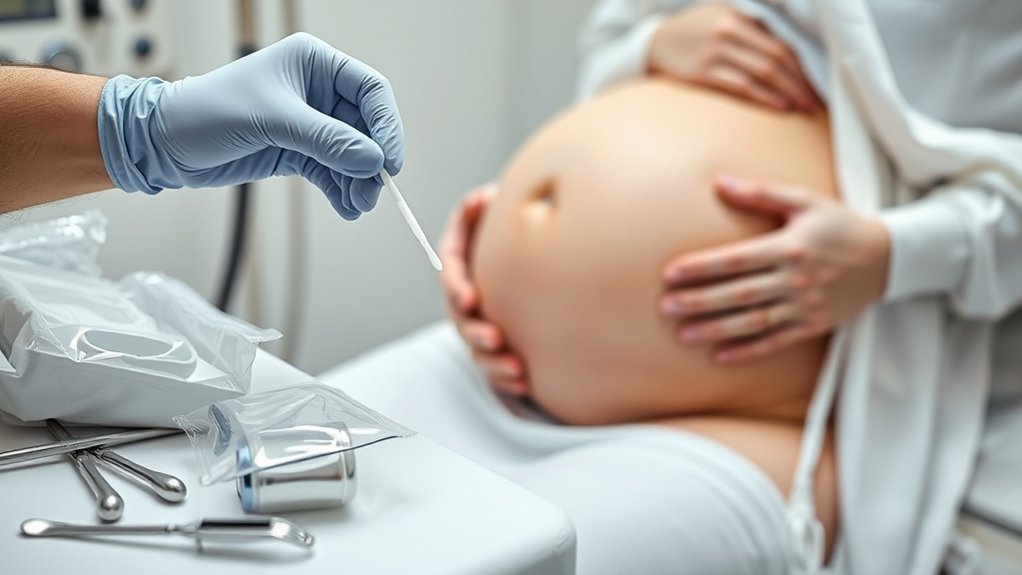
The GBS test in pregnancy is a simple swab of your lower vagina and rectum, usually done at 36 to 37 weeks. Your provider uses a sterile swab, and the process takes only a few minutes. If your test is positive, it means Group B Strep is present, not that you’re sick. Antibiotics during labor can greatly lower your baby’s infection risk, and there’s more to know about how it all works.
What Is the GBS Test in Pregnancy?
The GBS test in pregnancy is a routine screening done at about 36 to 37 weeks to check for Group B Streptococcus, or GBS, in your vagina and rectum.
This simple swab looks for GBS, a bacterium that often causes no symptoms in you but can create serious risks for newborns during delivery. About 1 in 4 pregnant people test positive, so a positive result is common and manageable.
If your test is positive, your care team usually recommends antibiotics during labor to lower the chance of passing Group B Streptococcus to your baby. This preventive step greatly reduces infection risk and supports a safer birth experience.
The swab is quick, painless, and part of standard screening endorsed by ACOG. Knowing your status gives you informed choice and helps you protect your newborns with evidence-based care.
When to Get Screened for GBS
You should get screened for Group B Strep in your third trimester, ideally between 36 and 37 weeks of pregnancy, because this timing gives your care team the most accurate information before delivery.
The American College of Obstetricians recommends this window for routine screening so healthcare providers can act promptly if Group B Streptococcus is present. About 1 in 4 pregnant women test positive, so GBS testing is a standard part of prenatal care, not a sign that anything is wrong.
Routine GBS screening is standard prenatal care, helping providers respond quickly if Group B Strep is present.
Even if you plan a cesarean, you still need to be screened for GBS, since labor and delivery can begin before surgery.
When you test at 36 to 37 weeks, your healthcare providers can help prevent GBS transmission with targeted measures that protect your baby.
This early, evidence-based approach supports safer birth choices and respects your body’s needs.
How the GBS Swab Is Collected
At your screening visit, your clinician collects the GBS swab with a sterile cotton swab by gently sampling the lower vagina and rectum; this quick test usually takes only a few minutes and isn’t painful. During pregnancy, a flocked swab may be used to improve specimen collection and release. You may feel brief pressure, but the process is painless and routine.
| Step | What you’ll notice | Why it matters |
|---|---|---|
| 1 | Swab touches the vagina | Gathers the needed sample |
| 2 | Swab touches the rectum | Improves detection of GBS |
| 3 | Sample goes to the lab | Supports laboratory analysis |
After collection, your sample goes to the laboratory for analysis, and results often return within 48 hours. If you receive a positive GBS test, your team will plan intravenous antibiotics during labor to lower newborn exposure risk. This straightforward GBS swab helps you make informed choices and protect your care plan.
What a Positive GBS Test Means
A positive GBS test means Group B Strep bacteria are present in your vagina or rectum and could be passed to your baby during birth. This result shows you carry Group B Streptococcus, not that you’re ill.
About 1 in 4 pregnant people test positive, which is why routine screening at 36 to 37 weeks matters. Most people with a positive GBS test have no symptoms, yet the finding guides care in labor.
Your team will plan intravenous antibiotics during labor to lower the risk of infection for newborns. Without treatment, the chance of a GBS infection in newborns is about 1 in 200; with treatment, it falls to about 1 in 4,000.
A positive result stays relevant throughout pregnancy, so preventive measures and close monitoring help protect your baby while keeping your birth choices centered and supported.
How Antibiotics Prevent GBS in Newborns
When a GBS test is positive, IV antibiotics during labor help protect your baby by lowering the chance that the bacteria will pass to the newborn. With routine screening, you and your team can act early against Group B Streptococcus and reduce the risk of GBS complications. Penicillin or ampicillin usually starts at least four hours before delivery, and this timing helps prevent GBS more effectively. If you test positive for GBS, your care team may also treat GBS in urine right away.
Additionally, ensuring adequate calcium intake is essential for maintaining overall health during pregnancy.
| Measure | Effect | Timing |
|---|---|---|
| Routine screening | Finds risk early | 36-37 weeks |
| IV antibiotics | Lowers transmission | Labor |
| Penicillin/ampicillin | Prevents infection | Before birth |
| Urine GBS treatment | Adds protection | As soon as found |
| Results | Fewer newborns with serious illness | Delivery |
This approach cuts the chance of early-onset GBS disease from about 1 in 200 to 1 in 4,000, helping newborns stay safer and supporting your freedom to choose informed, evidence-based care.
Frequently Asked Questions
Can I Do the GBS Swab at Home?
You can’t reliably do the GBS swab at home; ask your clinician about home testing only if they approve. Proper swab procedure, testing accuracy, risk factors, treatment options, and pregnancy timeline protect maternal health.
Does the GBS Test Hurt?
Usually, you won’t feel pain; the swab procedure may cause mild discomfort. Your test experience depends on anxiety factors. Use preparation tips, ask about pain management, consider alternative options, and follow medical advice for follow up care.
What Should I Avoid Before My GBS Swab?
Avoid douching, vaginal creams, tampons, and sexual activity before your swab; ask about antibiotics use. Keep normal diet considerations, personal hygiene, physical exertion, stress management, and hydration levels, and you’ll usually need no special prep.
Can GBS Go Away Before Labor?
Yes, GBS can disappear before labor, but you can’t assume it’s gone. Your healthcare provider may recheck testing frequency, review risk factors, discuss treatment options, preventive measures, symptoms awareness, transmission methods, and importance timing.
Will I Need Another GBS Test Later?
Yes, you may need another GBS test later; Medicare-style GBS screening guidelines usually repeat near 36–37 weeks. Your provider’ll review GBS risk factors, symptoms awareness, and post test follow up to protect maternal health, newborns.
Conclusion
Getting the GBS test in pregnancy helps you and your care team protect your baby before labor begins. If your swab is positive, why worry when antibiotics during labor can greatly lower the risk of infection? With timely screening and treatment, you can feel more prepared and supported. Talk with your provider about your results, your birth plan, and any questions you have so you can move forward with confidence.