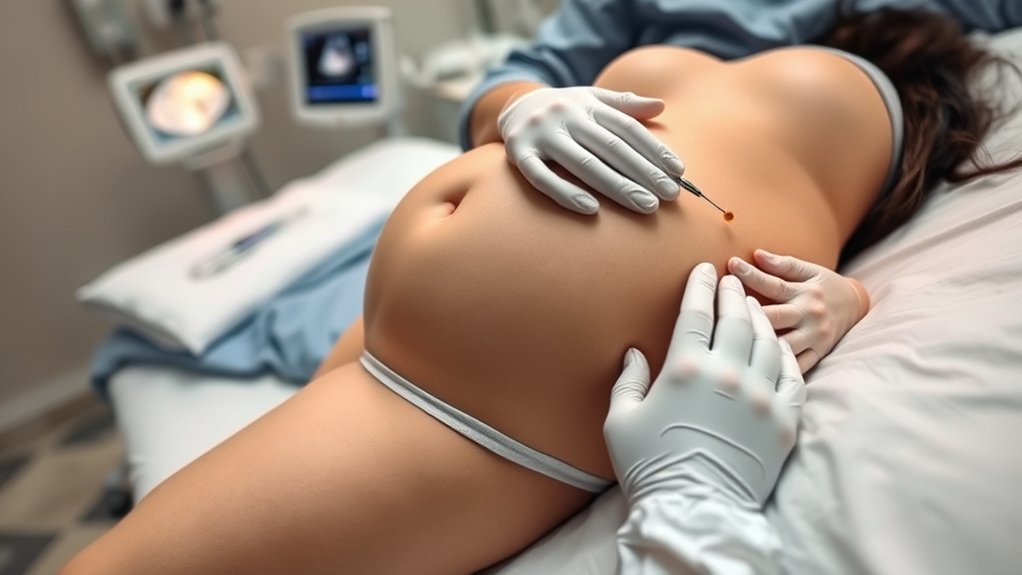
Amniocentesis is a prenatal test usually done at 15 to 20 weeks to check for genetic or chromosomal conditions. Before the procedure, your provider reviews risks, may ask you to drink water, and answers questions. During the test, ultrasound guides a thin needle into the amniotic sac to collect fluid. Afterward, you may rest, avoid heavy activity, and watch for bleeding or cramping. Results usually take days to weeks, and more details can help you prepare.
What Is Amniocentesis?
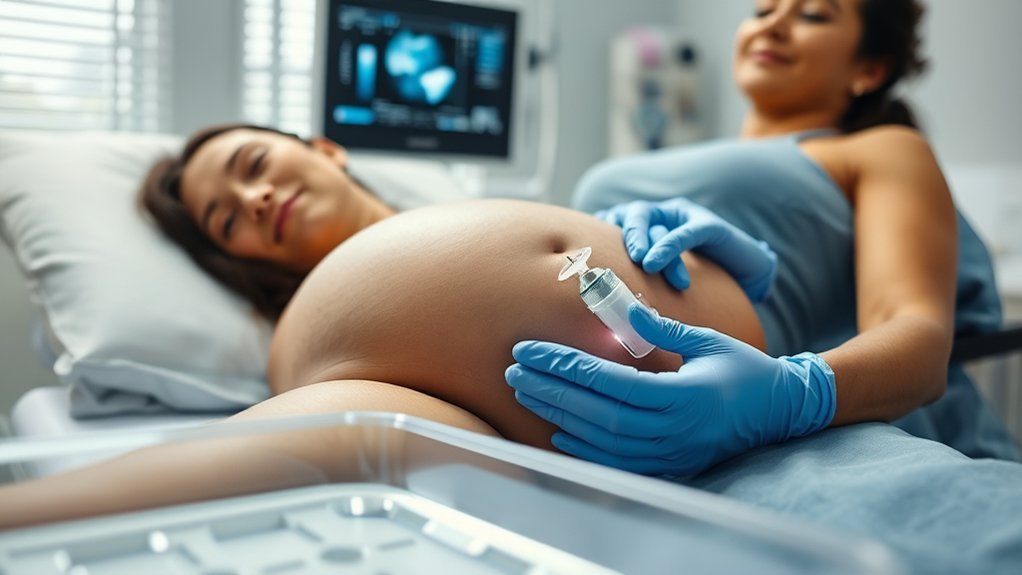
Amniocentesis is a prenatal diagnostic procedure in which a thin needle is used to remove a small amount of amniotic fluid from the uterus, usually between 15 and 20 weeks of pregnancy.
In this procedure, the fluid sample contains fetal cells, and clinicians can analyze it for genetic disorders, chromosomal abnormalities, and certain infections. You may hear it described as a highly accurate test, with about 99% accuracy for some conditions.
Like any invasive procedure, it carries a miscarriage risk, estimated at about 1 in 900. The sample may be tested quickly or sent for more detailed analysis, so results can take from 1 day to several weeks.
Like any invasive procedure, amniocentesis carries a miscarriage risk, and results may take from 1 day to several weeks.
Knowing what amniocentesis involves can help you make informed, autonomous decisions about your prenatal care. It gives you clearer information about your pregnancy while keeping the process medically focused, precise, and as reassuring as possible. Additionally, understanding the risks and benefits of amniocentesis is vital for making an informed choice.
Why Your Doctor May Recommend Amniocentesis
Your doctor may recommend amniocentesis when the potential benefits of getting precise information outweigh the small procedural risks. You may be offered this diagnostic test if you’re 35 or older, have a family history of genetic conditions, or received a prenatal screening test result that suggests increased risk.
It can also be advised when ultrasound findings raise concern, such as fetal abnormalities or soft markers. If a previous pregnancy involved a known genetic condition, amniocentesis can help you confirm or rule out a similar issue now.
In some situations, it also helps diagnose fetal infection or assess lung maturity before an early delivery, giving you clearer options.
- A quiet exam room, with the ultrasound screen glowing beside you
- A focused review of your family history and test results
- A careful discussion of benefits and the risks of amniocentesis
- A path to informed choices, with more control over your next steps. Additionally, your healthcare provider may discuss genetic disorder screening to help you understand potential outcomes.
What Amniocentesis Can Detect
When amniocentesis is performed, the fetal cells in the amniotic fluid can reveal important information about chromosomes and inherited conditions. You can learn whether your baby has genetic disorders such as Down syndrome, cystic fibrosis, or Tay-Sachs disease.
Laboratory testing also looks for chromosomal abnormalities, including extra, missing, or damaged chromosomes, through karyotyping and targeted genetic testing. If your care team needs a faster answer, rapid tests can screen for Down syndrome sooner, while full karyotype results usually take 2 to 3 weeks.
Amniocentesis can also assess lung maturity, which helps guide decisions if early delivery is being considered. In some cases, it can identify fetal infections, including TORCH-related infections, so your prenatal care team can respond appropriately. Additionally, understanding the risks and benefits of amniocentesis can help you make informed choices about the procedure.
The results won’t change your choices by themselves, but they can give you clear, evidence-based information so you can make informed decisions with greater confidence and autonomy.
How to Prepare for Amniocentesis

Before the procedure, your healthcare provider will explain how amniocentesis is done and review its risks and benefits with you so you can give informed consent. In health care, clear information helps you move forward with confidence.
Your care provider may advise a full bladder, so drink water beforehand unless told otherwise. You usually won’t need fasting or other special preparation.
Your care provider may advise a full bladder, so drink water beforehand unless told otherwise.
- Bring a support person for calm, steady reassurance.
- Write down questions to discuss before you arrive.
- Wear comfortable clothing that’s easy to adjust.
- Expect a local anesthetic plan if your clinician uses one.
The amniocentesis procedure is typically brief, and preparation focuses on understanding, comfort, and safety. Additionally, it’s important to note that chorionic villus sampling is an alternative prenatal diagnostic test that may be considered based on your specific situation.
Share any concerns openly so your care provider can address them directly. You deserve a process that respects your choices and supports your autonomy.
What Happens During Amniocentesis
During amniocentesis, you’ll lie back while ultrasound guides the clinician in locating your baby and confirming its position.
A thin needle is then inserted through your abdominal wall into the amniotic sac to collect about 18–20 mL of fluid.
You may feel mild cramping, but the procedure is usually brief and closely monitored for safety.
Ultrasound Guidance
Ultrasound guidance lets your clinician clearly visualize the fetus and the surrounding amniotic fluid so the needle can be placed accurately and safely. During the procedure, the transducer maps a clear route, supports precise needle placement, and guides continuous monitoring of fetal heart rate and movement.
This real-time view helps you stay informed and in control while reducing complications.
- A bright image of the fetus on the screen
- A calm sweep of the transducer across your abdomen
- A careful search for the safest fluid pocket
- Visual confirmation after fluid collection
The procedure usually takes 10 to 30 minutes, and ultrasound documentation follows to confirm successful extraction.
Needle Insertion
Once the safest fluid pocket has been identified, your clinician gently advances a thin needle through the abdominal wall and into the uterus under continuous ultrasound guidance.
You may feel brief pressure or mild cramping during insertion, but the procedure usually stays brief and controlled.
Ultrasound monitoring tracks the fetal heartbeat and movement throughout, helping your team confirm that the needle remains in the right place.
Local anesthetics aren’t typically used, so you can expect the sensation to be short-lived and clear.
The needle placement itself is precise, and the step is completed with steady, careful technique.
From start to finish, this part of the procedure usually takes only a few minutes, supporting safe access to the amniotic fluid for the next stage.
Fluid Collection
With the needle positioned in the safest fluid pocket, your clinician withdraws a small amount of amniotic fluid—usually about 18 to 20 mL—while ultrasound continues to track the fetus and the needle tip.
First, a few drops may be discarded to lower contamination risk, then the thin needle helps collect the sample for testing. You may feel mild cramping, but numbing medicine usually isn’t needed. This procedure typically lasts about 30 minutes, and your fetus’s heartbeat and movement stay under monitoring throughout.
- Clear ultrasound screen
- Steady hand guiding the needle
- Fluid moving into the vial
- A labeled sample sent to the lab
After collection, the amniotic fluid sample goes for analysis, and results usually arrive in 3 to 14 days, depending on the tests.
How Amniocentesis Is Done
Amniocentesis is usually done between 15 and 20 weeks of pregnancy and takes about 10 to 30 minutes.
During this amniocentesis procedure, you’ll lie back comfortably while your clinician cleans your belly and applies gel for ultrasound imaging. The ultrasound helps locate your baby and guides a thin needle through your abdomen into the amniotic fluid.
Your clinician usually discards the first 1 to 2 ml, then collects about 18 to 20 ml for testing. You may feel mild cramping as the needle enters and fluid is withdrawn, but the procedure is brief and controlled.
Afterward, your baby’s heart rate and movement are checked right away to confirm well-being. You can then rest for the remainder of the day, and acetaminophen can ease discomfort if needed. It’s important to monitor for any signs of severe pain or infection after the procedure.
Results are typically ready in 3 to 14 days, depending on the tests ordered.
What Are the Risks of Amniocentesis?
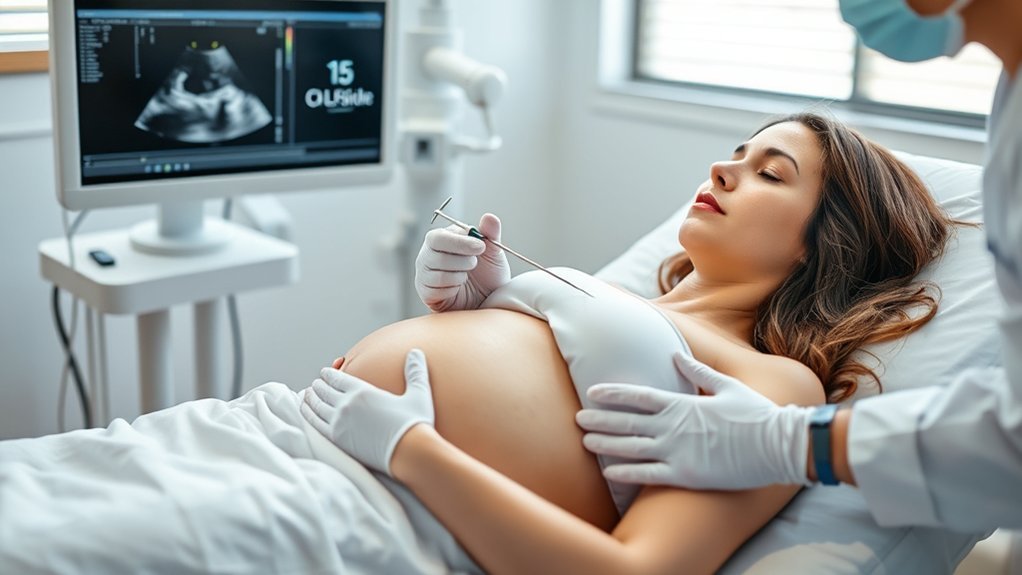
Amniocentesis carries a small miscarriage risk, about 1 in 900 procedures, so it’s generally considered a safe prenatal test.
You may also notice minor complications such as slight bleeding, amniotic fluid leakage, or brief cramping, and these usually resolve on their own or with simple measures.
Rarely, you could have infection or fetal injury at the insertion site, so your care team will review these risks and support you before and after the procedure. Additionally, the procedure can evoke emotional responses regarding the baby’s health, which is important to discuss with your healthcare provider.
Miscarriage Risk
Although amniocentesis carries some risk, miscarriage is a rare complication, occurring in about 1 in 900 procedures. You can view this as a small but real risk, and your healthcare provider should help you weigh it against the benefit of clear fetal testing.
Most patients experience no serious complications, and overall fetal loss averages 0.11%, with higher risk if you already have certain conditions.
- A fine needle guided by ultrasound
- A calm, brief clinic visit
- Mild cramping afterward
- Prompt follow-up if anything feels off
You may also notice a small chance of fluid leakage or vaginal bleeding, but these usually remain limited.
Ask direct questions before you decide, so you can move forward with confidence, autonomy, and informed choice.
Procedure Complications
Because every procedure has tradeoffs, it helps to understand the risks of amniocentesis before you decide.
With amniocentesis, the miscarriage risk is about 1 in 900, and minor procedure complications like spotting or cramping occur in about 1-2% of cases.
More serious risks can include amniotic fluid leakage, infection at the needle site, or rare fetal injury.
You may also feel emotional distress if results show abnormalities, so counseling matters.
Ask questions and request clear informed consent; your care team should explain how your maternal factors and history shape your risk profile.
This discussion isn’t about fear—it’s about informed, autonomous choice.
When you understand the facts, you can weigh benefits and risks with confidence and decide what’s right for you.
What Recovery Looks Like
After the procedure, you should rest for the remainder of the day to help limit discomfort and reduce the risk of complications.
In this post-procedure period, your body usually needs quiet support, not strain. Mild cramping or soreness at the needle site is common, and acetaminophen can help if your clinician approves.
Keep your movements deliberate, and avoid heavy lifting, strenuous exercise, and sexual intercourse for at least 24 hours. This monitoring phase helps you protect your recovery and preserve your options.
Watch for signs that need prompt care:
- Heavy bleeding
- Severe cramping
- Leakage of amniotic fluid
- Worsening pain or dizziness
If any of these occur, contact your healthcare provider immediately.
Most people recover smoothly after the amniocentesis procedure and resume normal activity soon. Your results may take several days, but this waiting period doesn’t change your need for careful rest today. Additionally, maintaining essential nutrients during recovery can support overall health and healing.
When You’ll Get Amniocentesis Results
You’ll usually get amniocentesis results in about 10 days to 3 weeks, although some rapid tests for specific chromosomal abnormalities can return in as little as 1 day. The timing depends on which analyses your sample needs, and your clinician will tell you what to expect. When your results come back, they’ll be reported as normal or abnormal, and you should schedule a follow-up to review the findings and any next steps. Understanding the risks associated with CVS can provide valuable context when discussing amniocentesis results and implications.
Result Timeline
Amniocentesis results usually take 10 days to 3 weeks, depending on the type of analysis performed. Your amniocentesis test results follow a clear timeline, so you can plan without feeling trapped by uncertainty.
Genetic screening for chromosomal abnormalities may return faster when the lab runs a targeted analysis, sometimes in 1 day. Full chromosome review often takes 2 to 3 weeks.
- A phone call from your clinic
- A message in your patient portal
- A quiet wait while the lab works
- A follow-up visit with your healthcare provider
Your healthcare provider can explain what’s pending, what’s final, and when you’ll hear next. If you need liberation from guesswork, ask about your expected timeline before you leave the clinic.
Test Type Impacts
The type of analysis ordered can change when you get your amniocentesis results. With amniocentesis, your prenatal test may return test results in 10 days to 3 weeks, depending on what the lab examines in the genetic material.
Rapid assays for conditions such as Down syndrome can deliver answers in about 1 day. Full karyotype testing, which reviews chromosome number and appearance, usually needs 2 to 3 weeks.
Your provider chooses tests based on the procedure used, and that choice shapes timing. Laboratories’ workload can also affect turnaround. If specialized genetic conditions need comparison with parental mutations, the invasive procedure may require extra processing time.
This range is normal and reflects careful analysis, not delay by default.
Next Steps After Results
Depending on the tests ordered, amniocentesis results usually come back in about 10 days to 3 weeks, though rapid screening for certain conditions, such as Down syndrome, may be available within a few days.
After amniocentesis procedures, you’ll wait for clear answers while your mind settles. Normal results suggest no detected genetic conditions. Abnormal results need discussion with your healthcare provider, who’ll explain what they mean and your options.
Contact your provider right away if you have pain, fluid leakage, fever, or bleeding. Follow-up care may include genetic counseling to help you understand the results and any pregnancy implications.
- A phone call from the clinic
- A calm office visit
- A genetic counseling session
- A plan for next steps
What Your Amniocentesis Results May Mean
Once your amniocentesis results are available, they can confirm or rule out genetic conditions such as Down syndrome, cystic fibrosis, and spina bifida with about 99% accuracy. Your amniotic fluid sample offers a diagnostic result, not just a screening test, so the accuracy rate is high. Normal findings mean no detected chromosomal abnormalities. Abnormal results require prompt review, genetic counseling, and possible follow-up testing to clarify the finding. Additionally, understanding the implications of Chorionic Villus Sampling can provide further context for your results and decision-making.
| Result | Meaning |
|---|---|
| Normal | No detected chromosomal abnormalities |
| Abnormal | Further discussion needed |
| Rapid test | Preliminary answer in days |
| Full karyotype | Complete results in 2–3 weeks |
| Next step | Plan care and support |
These results can guide pregnancy management and help you prepare for treatment, delivery planning, or newborn support. If you receive abnormal results, you don’t have to face them alone; clinical guidance and emotional support can help you make informed choices with clarity and dignity.
Frequently Asked Questions
What Not to Do Before Amniocentesis?
Don’t overeat, skip counseling, or take blood thinners before amniocentesis. Don’t ignore symptoms. Use amniocentesis preparation tips, discuss with partner, address common fears, and lean on emotional support strategies while understanding risks and post procedure symptoms.
Has Anyone Miscarried After an Amnio?
Yes—some people have miscarried after amnio, but it’s uncommon: about 1 in 1,000. You can discuss miscarriage risks, procedure safety, success rates, patient experiences, emotional support, and doctor recommendations to stay informed and steady.
How Many Days Should I Bed Rest After an Amniocentesis?
You should rest one day, then ease back over 24–48 hours. Follow post procedure care, use comfortable resting positions, prioritize hydration importance, follow activity restrictions, seek emotional support, and keep follow up appointments.
Can I Drive Myself Home After an Amniocentesis?
No, you shouldn’t drive yourself home after amniocentesis; arrange a ride. Driving considerations, Post procedure care, Pain management tips, Emotional support options, Follow up appointments, Risks and benefits all favor safety, rest, and support.
Conclusion
Amniocentesis gives you clear, clinically useful clues about your baby’s health. You’ve seen the simple steps, the small risks, and the usual recovery, so you can feel more prepared and less परेशान? no, we need clinical, reassuring. Let’s correct.
Amniocentesis gives you clear, clinically useful clues about your baby’s health. You’ve seen the simple steps, the small risks, and the usual recovery, so you can feel more prepared and less pressured. If your doctor recommends it, ask questions, follow instructions, and trust the process. With careful preparation and prompt follow-up, this precise procedure can provide peace of mind and practical prenatal information.